Inhalants & Volatile Substance Abuse
Help Stop Inhalant and Volatile Substance Abuse.
Every year an untold number of individuals die as a result of intentionally inhaling common, legal, everyday home, school and office products. The National Inhalant Prevention Coalition (NIPC) reports approximately 100 to 125 inhalant deaths per year, based on contacts with families of victims and media accounts.
Intoxicating Inhalants: The Problem
There has always been a problem with juveniles, teens and young adults misusing and abusing over the counter and prescription drugs. Yet, in this instance, we define the term, “drug”, as any mood or mind altering substance obtained and consumed or inhaled without the knowledge and legal consent of a prescribing licensed physician. This may include any household product when used contrary to manufacturer’s intended purpose. Misuse of inhalants and volatile solvents are especially dangerous to such extent a single use can and has resulted in sudden death for some Canadian youths.
As a parent, if inhalant use and abuse is a subject unfamiliar, in a moment you will understand why parents allow proper attention to this group of quirky substances and why the threat to users is especially serious in some communities. More to the point, this threat increases exponentially because it is highly likely several of these chemicals and/or chemical compounds are sitting in your home at present. Of course, this alone makes for the easy access since unlike alcohol, nicotine and cocaine, where acquisition and access are prohibited by law and potentially costly to acquire.
Inhalants Defined
Inhalants may be anything from gasoline, lacquers or spray paints, paint thinners, glue, compressed air, a chemical in whipped cream, a component of Sharpie markers, furniture polish, chemicals in pesticides and a thousand other common household products. These products typically contain any or all of three common chemicals: Toluene, fluorocarbons, and nitrous oxide.
 Manufacturers of lacquers and other materials routinely publish full disclosure statements warning those who work with or have contact with their product of dangers stemming from exposure. An actual example, of one such warning shown.
Manufacturers of lacquers and other materials routinely publish full disclosure statements warning those who work with or have contact with their product of dangers stemming from exposure. An actual example, of one such warning shown.
Just as we have stated in this article, so do manufacturers warn… death can result from misuse and prolonged exposure. Truth is this… anything in an aerosol and vapor form can ignite and potentially explode. Intentional misuse via inhalation and especially prolonged use is essentially the equivalent of a loaded shotgun and a death wish. Do not do it and tell your children not to and why – you may save someone’s life by sharing this information.
How Inhalants Enter the Body
Inhalants and volatile solvents enter the body much the same as oxygen -users breathe in through the mouth or via nasal passages. Inhaled chemicals quickly pass through the lungs and enter bloodstream, easily passing blood-brain barrier -a boundary human bodies possess designed to keep poisons from interrupting brain functioning. From this point, anything goes. There are, however, various stages users commonly report experiencing.
What Inhalants Do
Initial physical response to inhalants a user loses inhibitions and begins to feel “high”. This feeling of euphoria is actually a state of confusion within the body and mind. The “high”, or euphoria, begins sometimes within seconds or may take as long as a few minutes before the feeling initially occurs. Inhalant users have reported dizziness, nausea, vomiting and even loss of consciousness as side effects. Minutes later, a user may hallucinate. Once the high passes, solvents act much as depressant drugs or alcohol slowing down the body’s central nervous system.
Some users suffocate after becoming unconscious when “bagging”. Some experience hyper-sensations of being invincible that may result in an individual inadvertently taking their own life in an accidental death circumstance. Still other users have burnt to death because inhalants and solvents are highly flammable and may catch fire from sparks of a misplaced lit cigarette.
Inhalants Long Term Effects
If users do not die from volatile solvents and inhalants in short term, long-term effects are quite serious. Some examples: chronic nose bleeds, hearing loss and brain damage. Impaired functioning of vital body organs such as liver, kidneys, heart and lungs, as well as bone marrow. Most of these disorders never go away and continue to plaque users until death. (CPHA.ca)
Immediate Signs of Inhalant Use
According to Canada Public Health Association web page offering an overview on inhalants and solvents, the following are a few day after signs and examples of telltale signs parents should watch for. These symptoms include:
- Watery or bloodshot eyes
- Stomach ache or vomiting
- Bleeding or runny nose
- Diarrhea and abdominal pain
- Drooling and spitting
- Headache
- Dizziness
- Stains on fingers or hands
- Chemical smell on clothing, hair or breath
Source: CAPHA
Not For Human Consumption
Little oversight prevents a child or teen from purchasing these common household products. Police lack authority to police these type chemicals. No proof of age nor age requirement prevents kids from acquiring these chemicals taking them home and misusing them. Even though at least one product may result in instant and sudden death. This product is canned air used by many clerical workers as an office cleaning supply. Canned air is actually a mixture of chemicals heavier than oxygen in weight. Inhaling these chemicals has proven deadly in many cases.
Intoxicating inhalants have consequences when one develops dependence. Despite potential harms, intoxicating inhalants are available in most stores because legitimate uses out number official reports of deaths from misuse. When death occurs from misuse of inhaled volatile solvents it is difficult to directly link to actual cause unless there are witnesses on scene.
Indigenous Youth Inhalant Use
Studies of First Nations communities in Canada and United States suggest up to 60 percent of youth living on Indigenous lands use and abuse of chemical inhalants. Inhalants are inexpensive and almost anyone can buy them off the shelf at a local store. (NAHO). Some household products open to abuse include gasoline, Sharpies, paint thinner, air duster in a spray can, different types of glue, and others. A statistic published by Foundation for Drug-Free World states, 22% of inhalant abusers who died of Sudden Sniffing Death Syndrome had no history of previous inhalant abuse – they were first-time users (Drugfreeworld.org).
Ontario Student Drug Use and Health Survey
The Centre for Addiction Mental Health’s conducts an on-going study designed to assess youth drug use is an ongoing school survey that asks participating students about prior drug use in the previous year. This study, Ontario Student Drug Use and Health Survey or OSDUHS, is the longest ongoing study of its kind. To date, reported findings are based on 19 survey cycles conducted every two years since 1977.
In 2013, 10,272 students (63% of selected students in participating classes) in grades 7 through 12 from 42 participating school boards, 198 schools and 671 classes participated in the OSDUHS administered by the Institute for Social Research, York University. The 2013 survey concluded:
- a total of 3.4 percent of the students have or are abusing inhalants
- 2.4% of the males and 4.1% of the females
- Highest use of 7.6% by students in the 8th grade.
Further 2013 OSDUHS Survey results found a significant decrease in inhalants use for non-Indigenous youth (and 17 other drugs that were highly abused) from 1999 to 2013. For inhalants, glues and solvents a decline from 8.9% in 1999 to 3.4% in 2013 (OSDUHS). The survey found students reporting inhalant use in 2011 declined in 2013 for most provinces, while others showed no decline. Aboriginal communities are examples of those showing no decline. Moreover, according to participants, average age of initiation to inhalants and solvents is becoming increasingly lower now between the ages of 10 and 13. This places the median age of first inhalant experience at the tender age of 11.5. Of course, this factor alone is indicative of serious future issue since this youth demographic (persons under fifteen years of age) is the fastest growing segment of Canada’s overall population making up 5-6 percent. This may prove big trouble for Canada’s future healthcare system, economically speaking since two Indigenous communities have youth populations almost twice the national average. Do the math and realize 5-6 percent amounts to large numbers of at-risk youth.
In Northwest Territories “one person in five, or 21.4%, living in this territory are under 15 years of age, while only six persons in 100 (6.2%) are aged 65 and over. In Nanavut, 31.7% of the population are under 15 years of age”. A proportion almost twice Canada’s national average.
Imagine the damage that inhalants may inflict on human bodies before adulthood if inhalant use becomes habitual. For these and other reasons, Crime Stoppers urges teachers, parents, guardians and lawmakers to gain an understanding as to how to curtail Canadian youth inhalant problem. If left unchecked, this growing problem will reach pandemic proportions and most certainly place a future economic strain on Canada’s health care system in the future.
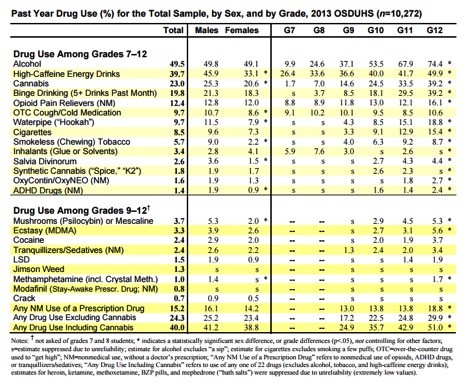
The following table published by Canada’s Centre for Addiction and Mental Health in 2013, offers an at a glance comparison of the above statistics including those regarding inhalant use by Canadian school children and teens:
Parents Not Enlightened to Child’s Inhalant Use
With such numbers widely reported, it is no wonder, at least one source calls it “startling” when the Partnership for a Drug-Free America reported in their 2002 Parent Attitude Survey (PATS) reports parents knowledge of a child’s drug use lags far behind at a ratio of 18:1. More to the point, 18 percent of teens (ages 12-17) reported having tried inhalants while only 1 percent of parents of teens believe their child has tried inhalants.
Further, the 2002 PATS reported most parents of school-aged children who discuss drugs with their child are less likely to discuss inhalants than marijuana or other drugs such as heroin, cocaine and crack. For example, 50% of parents discussed marijuana, 39% discussed heroin, cocaine and crack; while only 33% discussed inhalants.
Prevention Education Programs
In those communities with declining inhalant abuse rates there exists a direct link to the presence of prevention education programs, substance abuse treatment centers and adequately staffed clinical and social services. All undeniably absent in those other communities where use, abuse and addiction rates continue to climb. Teachers, community leaders and health care professionals tend to agree educational efforts empower youth to make the right decisions in life.
Teaching children and teens how misuse of common household chemicals like lacquers, gasoline, paints and glues or other household chemicals harm human organs such as lungs, kidneys, brain functionality, oral health. Or, how too often, misuse of inhalants leads to mental health issues for habitual users, it is highly likely most will elect to avoid experiential learning.
Advice for Parents
As a parent or guardian, lack of prevention education in schools and communities makes this conversation with children ultimately a parental responsibility; in the event you feel a bit intimidated by the thought of opening dialogue with your child – you are not alone. Remind yourself that the child’s life may depend on establishing an open line of communication in effort to enlighten children about probable hazards and cumulative harm to human bodies. This is especially true for parents of elementary age kids because inhalant and volatile solvent use now occurs at significantly younger age. Thus, making this type conversation a must.
We suggest a good starting point is explaining adverse bodily responses associated with inhalants such as gasoline and paint thinners. Perhaps even an impromptu role-playing where you ask your child to hold his or her breath for as long as possible which likely brings forth a certain gasping for oxygen in mere minutes. This suggestion is an ad hoc suffocation assimilation. Hopefully, this simulation is enough to convince vulnerable youth there are far better experiences to be had than dying from the misuse of gasoline, spray paints as inhalants, glues and solvents in pursuit of a quick high. In most instances, the attraction for most youth is in challenging the outside world, pushing and stepping on lines and boundaries relating to illicit drug experimentation.
If the thought of entertaining these conversations give you reason to pause, please visit any of the resources cited for additional facts and information relating to inhalant, glue and solvent abuse, substance abuse in general and youth suicide prevention.
Parents, youth and citizens can also contact your local Crime Stoppers agency or local law enforcement if you need information and/or assistance with an at-risk youth or substance abuser.
Resources:
- National Inhalant Prevention Coalition (NIPC).
- Canadian Public Health Association (CPHA).
- G. Roberts, World Youth Report, United Nations Economic and Social Council, In press.
- World Youth Report
- DrugFreeWorld.org
- Boak, A., Hamilton, H.A., Adlaf, E.M., & Mann, R.E. Centre for Addiction and Mental Health, 2013
- Foundation for a Drug-Free World, “International Statistics”.
- Statistics Canada. September, 2012. Catalogue no. 91-215-X. ISSN 1911-2408.